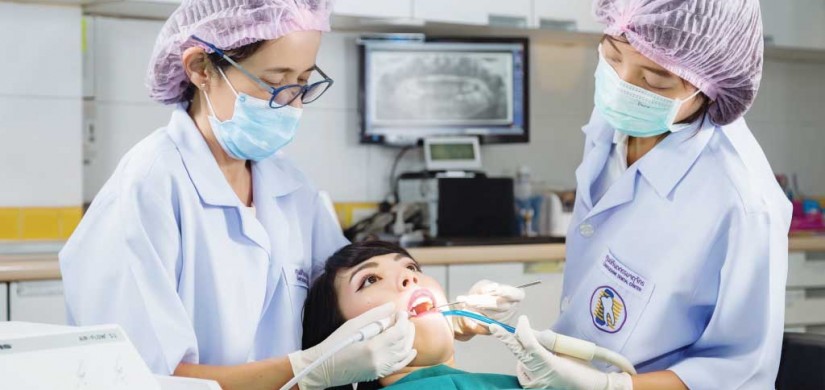
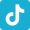Wisdom teeth are the last teeth to appear in your mouth, When your wisdom teeth are well-positioned and healthy, they are very important. Unfortunately, this does not generally happen. The extraction of wisdom teeth is necessary when they are prevented from properly erupting within the mouth. They may grow sideways, partially emerge from the gum, and even remain trapped beneath the gum and bone. Impacted teeth can take many positions in the bone as they attempt to find a pathway that will allow them to successfully erupt. These poorly positioned impacted teeth can cause many problems. When they are partially erupted, the opening around the teeth allows bacteria to grow and will eventually cause an infection. The result: swelling, stiffness, pain, and illness. The pressure from the erupting wisdom teeth may move other teeth and disrupt the orthodontic or natural alignment of teeth. The most serious problem occurs when tumors or cysts form around the impacted wisdom teeth, resulting in the destruction of the jawbone and healthy teeth. Removal of the offending impacted teeth usually resolves these problems. Early removal is recommended to avoid such future problems and to decrease the surgical risk involved with the procedure.
Immediately Following Wisdom Tooth Extraction
• The gauze pad placed over the surgical area should be kept in place for a half hour. After this time, the gauze pad should be removed and discarded.
• Vigorous mouth rinsing or touching the wound area following surgery should be avoided. This may initiate bleeding by causing the blood clot that has formed to become dislodged.
• Take the prescribed pain medications as soon as you begin to feel discomfort. This will usually coincide with the local anesthetic becoming diminished.
• Restrict your activities the day of surgery and resume normal activity when you feel comfortable.
• Place ice packs to the sides of your face where surgery was performed. Refer to the section on swelling for explanation.
Though nobody enjoys the thought of having teeth pulled, occasionally a tooth can crack, break or become so decayed in a way that cannot be repaired, others may have advanced periodontal disease . may need removal because they are poorly positioned in the mouth (such as impacted teeth), or in preparation for orthodontic treatment.
The removal of a single tooth can lead to problems related to your chewing ability, problems with your jaw joint, and shifting teeth, which can have a major impact on your dental health.
To avoid these complications, in most cases, our dentist will discuss alternatives to extractions as well replacement of the extracted tooth.
After Tooth Extraction
After tooth extraction, it’s important for a blood clot to form to stop the bleeding and begin the healing process. Bite on a gauze pad for 30-45 minutes immediately after the appointment. If the bleeding or oozing still persists, place another gauze pad and bite firmly for another 30 minutes. You may have to do this several times to staunch the flow of blood.
After the blood clot forms it is important to not disturb or dislodge the clot. Do not rinse vigorously, suck on straws, smoke, drink alcohol or brush teeth next to the extraction site for 72 hours. These activities may dislodge or dissolve the clot and hinder the healing process. Limit vigorous exercise for the next 24 hours, as this increases blood pressure and may cause more bleeding from the extraction site.
After the tooth is extracted you may feel some pain and experience some swelling. An ice pack or an unopened bag of frozen peas or corn applied to the area will keep swelling to a minimum. Take pain medications as prescribed. The swelling usually subsides after 48 hours.
Use pain medication as directed. Call our office if the medication doesn’t seem to be working. If antibiotics are prescribed, continue to take them for the indicated length of time even if signs and symptoms of infection are gone. Drink lots of fluids and eat nutritious, soft food on the day of the extraction. You can eat normally as soon as you are comfortable.
It is important to resume your normal dental routine after 24 hours. This should include brushing and flossing your teeth at least once a day. This will speed healing and help keep your mouth fresh and clean.
After a few days you should feel fine and can resume your normal activities. If you have heavy bleeding, severe pain, continued swelling for 2-3 days, or a reaction to the medication, call our office immediately.
A torus is an outgrowth of bone that is perfectly normal to develop, though not everyone develops tori. These excess bone growths may develop in either arch and may be a nuisance if they interfere with a dental appliance, your oral hygiene, or the space for your tongue.
The torus of the palate, or roof of the mouth, is known as the torus palatinus. The torus of the lower jaw is referred to as the torus mandibularis. You may develop tori due to your genetics or due to environmental changes like a local irritation, bruxing or grinding your teeth, or teeth that are in malocclusion, also known as an uneven bite.
While most tori are benign and do not require treatment, some tori may irritate you and require surgical removal or reshaping. Reasons for tori reduction include:
1. Accommodating upper or lower complete or partial dentures and provisional dentures.
2. Making better access for the mouth to be self-cleansing.
3. Creating better access for personal oral hygiene.
Depending on what caused the torus to develop, it may recur. The growth is usually slow and there is a small chance that retreatment may be necessary.
Missing teeth over a period of time can cause your jaw bone to atrophy, or resorb. This often results in poor quality and quantity of bone suitable for the placement of dental implants as well as long term shifting of remaining teeth and changes to facial structure. Most patients, in these situations, are not candidates for dental implants.
Fortunately, today we have the ability to grow bone where it is needed. This not only gives us the opportunity to place implants of proper length and width, but it also gives us a chance to restore functionality and aesthetic appearance.
Major Bone Grafting
Bone grafting can repair implant sites with inadequate bone structure due to previous extractions, gum disease, or injuries. The bone is either obtained from a tissue bank or your own bone is taken from the jaw, hip or tibia (below the knee). Sinus bone grafts are also performed to replace bone in the posterior upper jaw. In addition, special membranes may be utilized that dissolve under the gum to protect the bone graft, as well as encourage bone regeneration. This is called guided bone regeneration, or guided tissue regeneration.
Major bone grafts are typically performed to repair defects of the jaws. These defects may arise as a result of traumatic injuries, tumor surgery, or congenital defects. Large defects are repaired using the patient’s own bone. This bone is harvested from a number of different areas depending on the size needed. The skull (cranium), hip (iliac crest), and lateral knee (tibia), are common donor sites. These procedures are routinely performed in an operating room and require a hospital stay.